Candida auris is a rapidly emerging fungal infection with high morbidity and mortality rates.

Candida auris (C. auris)
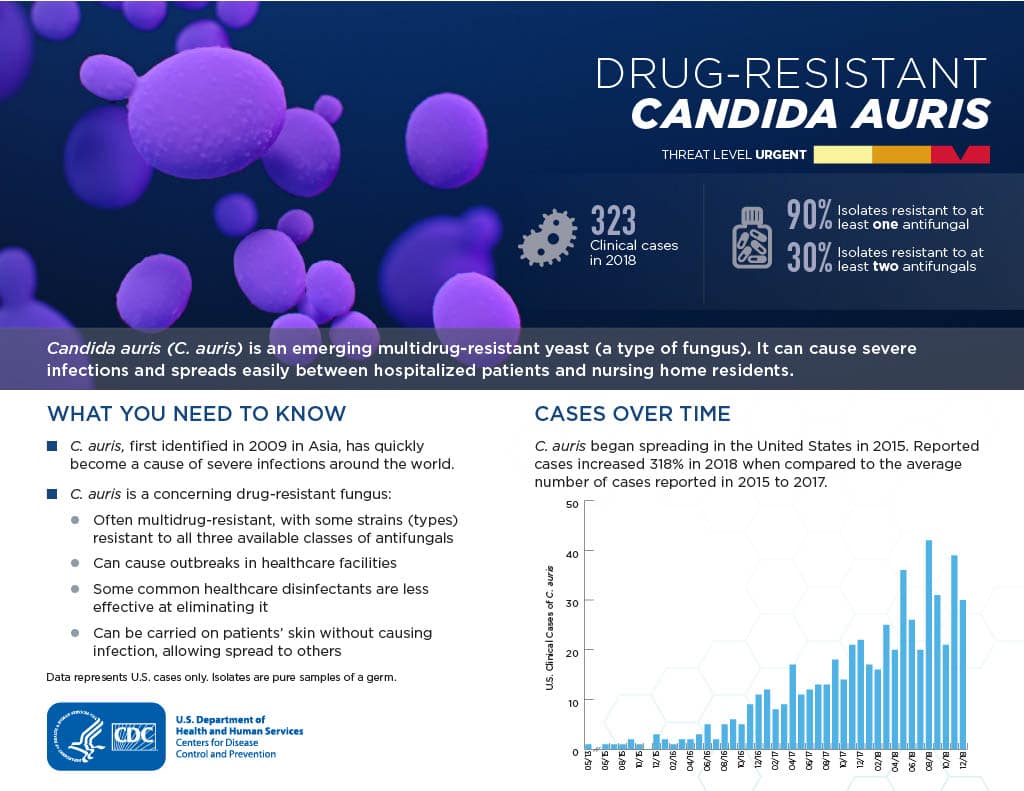
C. auris is a multi-drug resistant fungal (yeast) infection that exists in multiple geographic locations with a wide range of genomic diversity.
In 2016, the U.S. Centers for Disease Control and Prevention issued a Clinical Alert and classified C. auris as a Global Health Threat.
Due to several factors, including:
- Increased hospitalizations,
- A refocus of hospital infection prevention and control efforts, and;
- A reduction in screening,
C. Auris cases spiked during the COVID-19 pandemic, increasing from 13 reported cases by 2016 to more than 1,000 reported clinical cases in 2021.
A troubling cause for the increased case count may have been identified--a pan-resistant strain of C. auris invading U.S. healthcare facilities.
According to a 2021 article published by Healio;
A new report provides the first evidence that pan-resistant strains of Candida Auris may have been transmitted in U.S. hospitals, researchers said.
The report, published this week in MMWR, details two independent clusters of pan- or echinocandin-resistant C. Auris cases among patients with overlapping inpatient exposures and no echinocandin use.
The cases were detected between January and April of this year in Washington, D.C., and Texas.
Report suggests transmission of pan-resistant C. auris strains in US hospitals
Additionally, C. auris:
- Has a mortality rate of 30 to 60%.
- Is highly persistent, surviving for several weeks on common non-porous facility surfaces.
- Resistant to common disinfectants.
- Can spread from contaminated patients without an active infection.
- Poses a significant transmission risk to facilities and occupants during healthcare facility transfers.
- Is highly transmissible, and;
- Rapidly regrows within four hours of facility decontamination.
Infection Prevention and Control Measures
Preventing the spread of Candida auris requires enhanced infection prevention and control measures.
Environmental cleaning with a commercial-grade soap-based detergent must precede disinfection efforts.
Only disinfectants listed on the U.S. Environmental Protection Agency's List-K or List-P should be used to treat surfaces for Candida auris contamination, and only in accordance with the product manufacturer's instructions.
According to the EPA:
C. Auris is a fungus that can cause severe infections and spreads easily between patients.
C. Auris infections tend to occur in health care settings and can be resistant to antifungal drugs.
Prior to these products being registered, there were no antimicrobial pesticides registered specifically for use against C. Auris.
A product’s effectiveness can change depending on how you use it.
Disinfectants may have different directions for different pathogens.
Follow the label directions for C. Auris, including the contact time.
List P: Antimicrobial Products Registered with EPA for Claims Against Candida Auris
Additionally, follow standard hand hygiene practices that include the use of alcohol-based hand sanitizer after washing or instead of soap and water when the hand is not visibly soiled.
Issues With Rapid Recontamination
Increasingly, C. auris contamination has demonstrated rapid regrowth within hours of cleaning and disinfecting a room, underscoring the need for newer decontamination methods that complement enhanced cleaning and infection prevention and control practices.
Environmental services (EVS) staff completed daily patient room cleaning and disinfection, which included wiping down high-touch surfaces with hydrogen peroxide wipes, at an acute-care hospital and skilled nursing facility in Chicago and five skilled nursing facilities in Orange County, California.
Four hours later, researchers took samples from high-touch surfaces in the cleaned rooms, then repeated these samples after eight and 12 hours.
The samples revealed surfaces close to the patient were commonly re-contaminated with C. Auris only four hours after cleaning, including the overbed table (24%), bed handrail (24%), and remote/call button (19%).
However, samples taken outside of patient rooms, such as at the nursing station and on equipment carts, rarely detected C. Auris.
Frequent Cleaning Has Little Effect on Pathogen Found in Hospital Patient Rooms
A promising alternative mitigation strategy may be UV-C lighting.
According to research published by the National Institutes of Health;
[Candida auris] is responsible for several outbreaks within healthcare facilities, where it can be found on hospital surfaces and patient care devices.
Spread from these fomites may be prevented by improving the decontamination of hospital surfaces.UV-C decontamination may constitute an effective adjunct to routine room cleaning.
A maximal effect of C auris killing was found after 30 minutes of UV-C exposure at 2 m. With half the time or twice the distance, the efficacy strongly diminished to ~10 and ~50 fold, respectively. At suboptimal exposure times and distances, the C auris strains from Japan/Korea were more sensitive to UV-C killing than C auris strains originating from Venezuela, Spain and India.
Killing of Candida auris by UV-C: Importance of exposure time and distance
References & Resources
- Candida Auris
- Candida Auris Disinfection Best Practices
- Infection Prevention and Control for Candida Auris
- Tracking Candida Auris
Takeaway
Reported cases of Candida auris are increasing at an alarming rate.
Decontamination requires special training, protective equipment, and disinfection products.
Only experienced personnel should be allowed to decontaminate rooms suspected or known to be contaminated with Candida auris to avoid probable transmission.
Custodial teams outside of large healthcare facilities are likely ill-prepared and equipped to address the challenge of Candida auris facility contamination.
Outsourcing is a proven method for onboarding skilled service providers equipped with the latest training, processes, and technologies for a fraction of the price of maintaining a comparable service in-house.
Contact us today and discover why Vanguard Cleaning Systems® is the Standard of Clean® for businesses throughout Northwest Arkansas, Missouri, and Oklahoma.
In Oklahoma, dial 918-960-4450
In Arkansas, dial 479-717-2410
In Missouri, dial 417-812-9777

You must be logged in to post a comment.